Our nails and hair are unique parts of our bodies as despite being dead tissue, they play a huge role in enhancing or maintain standards of beauty. Our nails protect the fingertip and tissues from injuries while enhancing the precise movements of distal digits but are also cursed with many diseases and ailments including serious infections. The most of common of these are fungal or yeast infections resulting in Onychomycosis. Without suitable nail fungus treatment, the nail plate may separate from the nail bed, causing serious pain and injury.
Table of Contents
Nail Diseases & Infection Fungal or Yeast Infection
A fungal or yeast infection which results in Onychomycosis can invade through a tear in the proximal and lateral nail folds as well as the Eponychium, or cuticle. This type of infection is characterised by Onycholysis (nail plate separation) with evident debris under the nail plate. It normally appears white or yellowish and may also change the texture and shape of the nail. The fungus digests the keratin protein that makes up the nail, causing the changes in colour and texture. As the infection progresses, organic debris accumulates under the nail plate, often discolouring it. Other infectious organisms may be involved and if left untreated, the nail plate may separate from the nail bed and crumble off.
What are the symptoms of fungal infections of the nails?
At the start, there are usually no symptoms. Later the nails may become so thick, they start to hurt when they press against the inside of a shoe. Due to their thickness, they are often hard to trim. The look of an infected nail, particularly a fingernail, may cause embarrassment. The abnormal nail can damage socks and tights as the sharp or outthrust edges of the nail tear the fabric and may cut into the adjacent skin. Fungal infections can also spread to adjacent skin; it may itch, crack, form a blister or appear white, especially between the toes. What do fungal infections of the nails look like? Fungal infection of a nail usually starts at its free edge and then spreads down the side of the nail towards the base of the cuticle. Eventually, the whole nail may be involved. The infected areas turn white or yellowish and become thickened and crumbly. Less common are nails with white areas on the surface, The most common areas affected by fungal infections are the big and little toes. Sometimes, especially in those who carry out regular wet work such as housewives or cleaners, the skin around the fingernails becomes red and swollen. This is called paronychia and can allow an infection to get to the nail.
How are fungal infections of the nail diagnosed?
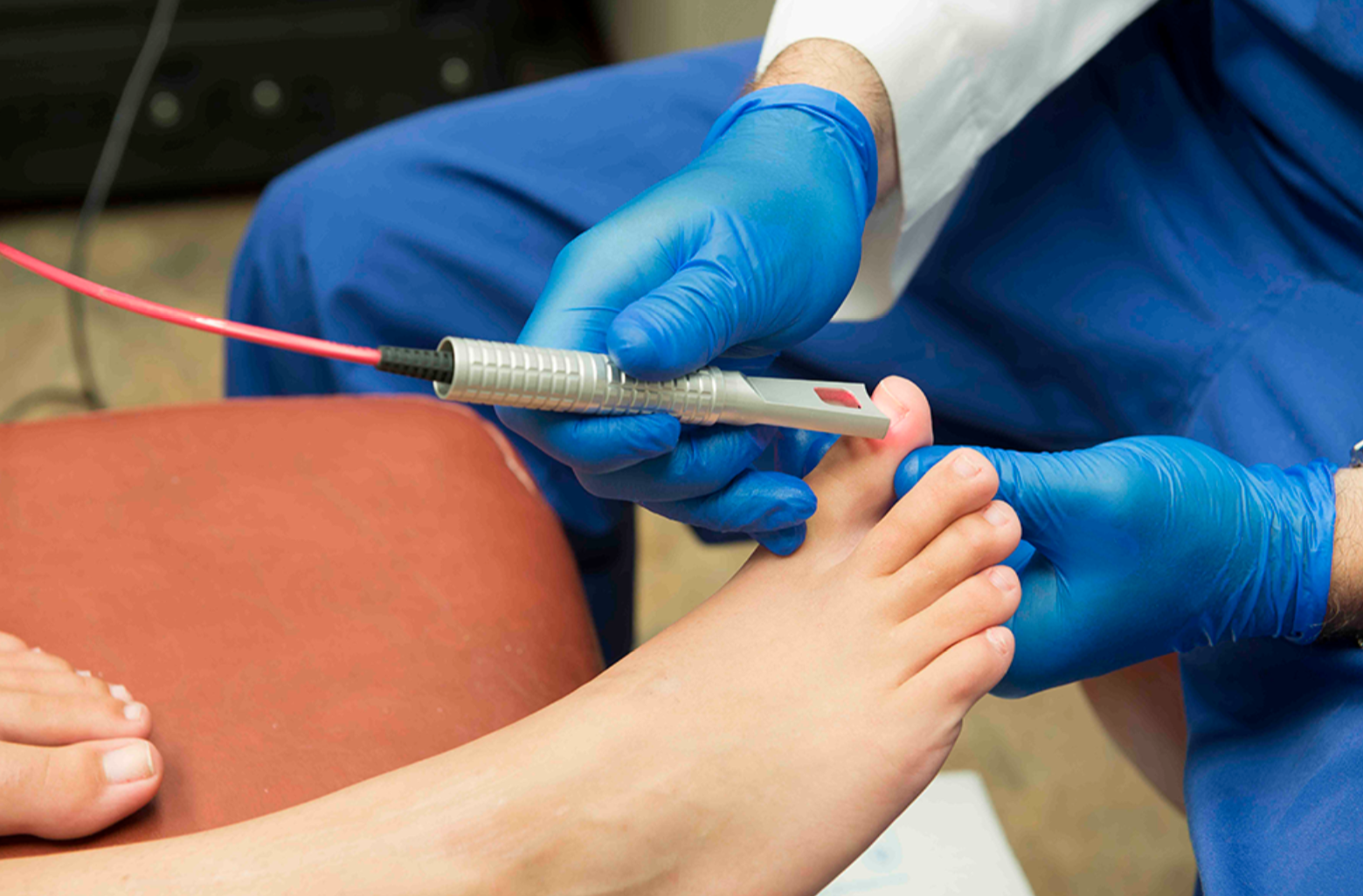
Fungal nail infections are usually diagnosed clinically even in a children’s foot clinic. Your doctor may take a small sample piece from the abnormal nail and send it to the laboratory to check if fungus can be seen under the microscope or grown in culture (this takes several weeks). Sometimes, repeated samples may be required. Many nail problems can look like a fungal infection, for example, the changes seen in psoriasis, after a bacterial infection or an old injury. Antifungal tablets may have a limited effect as there are many different types of fungal infections. Optimal treatment can depend on identifying the right fungus in order to ensure the right medication is used; it can take several weeks to get culture results.
How can fungal infections of the nails be treated?
Fungal infections of the nail do not clear up by themselves, but not all of them need treatment. Some people with infected toenails are not bothered by them at all. In that case, they can sometimes be left alone, though the patient should remain cautious and avoid spreading the infection to other parts of their body or other people. On the other hand, infected nails that are embarrassing or uncomfortable are usually treated. For people with underlying chronic conditions such as diabetes or suppressed immune systems, it is critical to treat fungal infections immediately as their bodies are extremely susceptible to further infection that can eventually be fatal.
The treatment aims to get rid of the fungus, returning the nail to normal. However, if the nail has been infected or damaged, the damage will remain. In severe cases, the nail may have to be removed and the surrounding area treated with antifungal medication in order to ensure that the treatment is complete. Nail infections caused by moulds and yeasts can be very resistant even to the best fungal nail treatments in Singapore.
Treatments applied to the nail (topical treatments)
Fungal treatments applied to the nail work less well than those taken by mouth. They are most effective if the infection is treated at an early stage. The treatments used most often are amorolfine nail lacquer and tioconazole nail solution. Alone, they may not be able to clear the deeper parts of an infected nail, though regular removal of abnormal nail material with clippers or filing can help with this. Used in combination with an antifungal remedy taken by mouth, they increase the chance of a full recovery. Such treatments may have to be used for a period of 4 to 12 months before a response is noted. The course of treatment is shorter for fingernail infections. The cure rate with topical agents alone, is low, approximately 15-30%. Topical treatments are safe though side effects such as local redness and irritation can occur.
Treatment by mouth (oral treatments)
1. Griseofulvin has been used for many years and is the only one of the three medicines licensed for use in children. It is only absorbed fully if taken with fatty foods (e.g. dairy products and milk), and long courses of treatment are usually needed (6 to 9 months for fingernails, and up to 18 months for toenails). Even so, only about three-quarters of infected fingernails and one-third of infected toenails will clear up.
Relapses are common.
2. Terbinafine and itraconazole have largely replaced griseofulvin. They work better and much more quickly, although only about 50% of nail infections are cured. Terbinafine should be considered as first-line treatment for dermatophyte fungi, which is the cause for the condition known as athlete’s foot. It is taken daily for 6 weeks for fingernail infections and 12-16 weeks for toenail infections.
3. Itraconazole is effective in treating dermatophytes; it is also useful for treating other fungi such as yeasts. It is often given in bursts for one week every month – because it is deposited into the cuticle of the nail and continues to be effective for a few weeks. Two of these weekly courses, taken 21 days apart, are usually enough for fingernail infections and three for toenail infections.
4. Fluconazole can be effective for Candida fungal infections. It is currently not licensed for fungal nail infections. It appears to be less effective than itraconazole and terbinafine but remains an alternative if someone is not able to tolerate these two medications.
Are there any side effects from the treatments?
Oral treatments are more likely to cause side effects than topical ones. Terbinafine occasionally causes a potentially severe allergic reaction that can make some skin conditions worse or even permanently affects one’s sense of taste. Itraconazole should not be taken if you are on certain medications. Your doctor will advise you about that. Both terbinafine and itraconazole can affect the liver, and your foot pain specialist in Singapore may arrange for blood tests to ensure that this medication is suitable before and during your nail treatment.
If you are looking for a nail fungal treatment in Singapore, visit our website today and let our experts help you with your problems.